Telemedicine Companies in India are at boom because of the increasing concern towards satisfaction of patients. Here we are going to discuss about the complete guide of Telemedicine and how to develop a telemedicine app.
Table of Contents
ToggleWhat is Telemedicine?
Telemedicine is the use of medical information exchanged from one location to another utilizing electronic communications to make the better health status of a patient. Telemedicine provides a growing variety of software and services that use two-way video, e-mail, mobile phones, wireless devices and other types of telecommunications technology.
Starting over forty years ago with hospital experiments providing services to patients in remote areas, the use of telemedicine has expanded exponentially and is now being incorporated into the daily operations of hospitals, specialty divisions, home health agencies, private physician’s offices, as well as consumers ‘homes and workplaces.
Telemedicine is not a separate medical discipline in its own right. Telemedicine related products and services are also part of a broader commitment by health-care institutions in either information technology or clinical care delivery. In fact in the reimbursement fee structure, generally no difference between on-site and those provided services by telemedicine, and often no separate coding needed for remote service billing.
How to develop a telemedicine app
Telemedicine app development steps are divided into many parts. Here is all steps are given by which you will learn how to build a Telemedicine Platform:
#Step 1: Business analysis
This step enables you to assess the market for your app and identify the persona of your customer, which will identify your target audience. The foundation of your approach should be market analysis. Your audience has issues, and those issues are solved by your product. Knowing who your client is will also allow you to successfully market your app after launch.
#Step 2: Design
The design of the user experience is the most important feature of the entire stage of app design. Many developers come up with excellent app ideas and create apps that perform very well from a technological point of view, but fail because the user experience is out of contact with the target audience.
#Step 3: Development
Corresponds to the coding phase of the app. The phase can focus on providing the first version of the app with key features to release it more rapidly to the market and then scale the project further with the next versions. Alternatively, a completely featured telemedicine program can be deployed at once, albeit at higher prices.
#Step 4: Quality assurance and UAT testing
Processes that ensure the telemedicine application’s high-end efficiency, output, and proper functioning.
A team of needed tech specialists-iOS and/or Android telemedicine app developers, back-end developers, and QA engineers-are allocated by the software development vendor.
#Step 5: Security checks
Compulsory and requires security testing for telemedicine applications.
#Step 6: Deployment
Finally, it’s time to move it to a live environment and into the app stores where users can download it once the app has been created. Release of the app to app stores and search optimization of app store profiles.
#Step 7: Maintenance and support
Per year, iOS and Android receive updates. To ensure that it continues to have the best user experience, it is necessary to update the app appropriately, Including bug fixes, enhancements, and current function tweaks.
Types of Telemedicine
There are three major forms of telemedicine including store-and-forward, remote monitoring and digital services in real-time. Each of these has a valuable role to play in overall healthcare and can offer measurable telemedicine benefits for both Clinic Staff and patients if properly used.
#1 Store-and-Forward” Practices
Store-and-forward telemedicine surpasses the need for the medical practitioner to meet in person with a patient. Instead of this, when obtained from the patient, data such as medical images or bio-signals can be sent to the specialist when appropriate. This practice is common in the dermatological, radiological, and pathological medical fields.
This technique may save time with proper planning and treatment, and allow medical practitioners to serve the public more fully with their services. This depends, though, on a background report and written facts or photographs rather than a physical examination that may cause misdiagnosis like complexity.
#2 Remote Patient Monitoring
Remote monitoring also known as self-monitoring or self-testing uses a variety of technology tools to remotely monitor a patient’s health and clinical signs. This is used widely for chronic disease control, such as cardiovascular disease, diabetes mellitus, and asthma.
Remote monitoring advantages include cost reduction, more frequent monitoring and greater patient satisfaction. There is a possibility that the tests conducted by the patients themselves might be unreliable, but the findings are usually considered to be comparable to the tests performed by the professionals.
#3 Real-Time Telemedicine
Interactive services may provide direct care to patients needing medical attention. There are many different media for this purpose are used, including television, internet, and home visits. A medical history and consultation about presenting symptoms can be undertaken, followed by assessment similar to those usually conducted in face-to-face appointments.
Teleneuropsychology is an example of this type of telemedicine which includes neuropsychological consultation and phone assessment with patients who have a cognitive disorder, or are suspected to have one. Standard evaluation techniques are implemented through video technology to assess the patient. A 2014 study found that this approach offers a viable and effective alternative to conventional in-person consultations, although it was noted that it is important to maintain quality standards and administration.
Read Also: Telepsychiatry- Mental Healthcare from Distance
Telenutrition is a way to use a Skype-like network to hold a diet therapy session entirely over the phone. From the safety of your home, you can undergo a nutrition therapy session. Telenutrition is the best choice for you if you live outside Warrenton, in remote areas or if you think this platform suits your lifestyle better.
Telepharmacy allows patients to seek prescription advice when direct contact with a pharmacist can not be made. This allows tracking of drugs, and advice can be given to patients over the phone. Based on the legislation, refill authorization can be provided to allow patients to receive medication regularly when appropriate.
Teledentistry can make dental care more accessible. It allows the dentists to meet patients with oral health needs in real-time. Teledentistry eliminates travel time, reduces the cost of transportation, and minimizes time off work or school.
Read Also: What kinds of Features, telemedicine app should have?
Advantage of Telemedicine for Patient:
1. Telemedicine boosts access to care
Travel and distance between care and patient providers can limit direct access to care. Fortunately, telemedicine overcomes geographical barriers to all healthcare, especially for specialized providers. Telemedicine mainly benefits patients belonging to rural geographical locations where there are no specialists or clinics.
2. Less Time in the Waiting Room
If you consult your doctor through telemedicine technology, you save your time by standing in a queue or looking at old magazines or newspapers in the doctor’s office.
3. More Accessible and Convenient Patient Care
The Cisco global survey shows that around 74% of patients offer easy access to all healthcare services. Through virtual care, it becomes easier for doctors to provide their patients with simple and on-demand care without involving much cost or wasting a lot of time and energy. Certain patients who live in rural and remote locations or people who do not have time to visit a hospital can access it virtually. Smartphone apps, online management systems and Video conferencing easily connect more people or patients with healthcare experts than ever!
Read Also: Questions to ask your Telemedicine Vendor
4. Extended Specialist and Referring Physician Access
Through the telehealth application, patients in remote or rural areas can access specialists easily and conveniently. In the United States, for 100,000 rural patients, there are about 43 specialists available. Due to fewer specialists, the patients have to wait for a longer time and have trouble accessing a particular disease. Telemedicine gives easy access to several specialities. In case your patient needs, you can recommend your patients to different physicians, regardless of the location.
5. No transportation costs or time
Since you can now see and talk to your healthcare expert on a mobile phone or through a computer, it saves much of your money on parking, public transportation, and gas. Additionally, you do not have to invest traveling time or the risk of striking into traffic jams, which can complicate the conditions as you can be late for your appointment and then work.
6. Telemedicine improves patient engagement and satisfaction
Telemedicine makes it more convenient and easier for patients to remain healthy and engage in overall healthcare. Patients want their healthcare providers to provide complete care, flexibility, and convenience when required!
7. No need for time off from work
Talking about the work, video visits eliminate the need to take any time off. You can schedule your doctor’s visit before, after work, or during lunch break. This ensures that you take continuous follow-ups without missing your work or wasting your time standing in lines to get your health checkup done.
Read Also: What Are The Benefits Of Telemedicine App In Healthcare Industry?
8. Better Patient Care Quality
Telemedicine follows a patient-centric approach, like an improved timeliness of care. This is important for the patient’s quality care. Through real-time urgent care consultations, patients can address all health concerns quickly and learn about different treatment options. According to a new study by researchers, telemedicine patients have less chance of developing anxiety, stress and depression and around 38% fewer hospital admissions.
9. Minimizing the spread of infection
Visiting any healthcare center means you are getting closer to infected people. People who have a weak immune system or carry some viruses or diseases are particularly dangerous for them. Through telemedicine technology, there is no need to visit the doctor’s office, which minimizes the chances of developing an infection during your visit to the doctor.
10. Convenience
Telemedicine allows people to access care in the comfort and privacy of their own home. This may mean that a person does not have to take time off of work or arrange childcare.
Technical Infrastructure Requirements of Telemedicine
HIPAA Compilent Telemedicine software has become the valuable medical software for health providers, especially in rural areas. A technical infrastructure requirement varies depending on the particular telehealth services of the organization, but some of required telehealth programs are common such as:
- Broadband internet access: Sufficient internet speed must need for the telehealth services. Sufficient bandwidth must be needed to transmit video and audio data.
- Imaging peripherals or technology: All devices act as the telehealth backbone! They allow people from remote distances or who live in rural areas to get immediate healthcare services, even if they are several kilometers away.
- Access to support people: To take care of the overall efficiency, technical support people must be shared across different collaborating companies. Technical support staff members can help answer questions about telemedicine programs.
- Staff training: Training your staff is vital to using telehealth technology efficiently, which can be time-consuming. It is best to consider the changes in the workflow and train your staff accordingly.
Telemedicine Clinical Guidelines
Although the industry is still a long way from meeting and fulfilling the standard set of guidelines meant for telemedicine, the American Telemedicine Association has established several potential guidelines for different specialities based on thousands of surveys and research studies conducted.
1. When to prescribe?
Prescription is accepted only for live video telemedicine sessions where replacing the visit with an in-person examination is possible. If the healthcare professional already has a relationship with you, prescribing can also happen for telephonic consultations.
2. When to prescribe
Prescription is acceptable for live video telemedicine sessions, where the visit can replace an in-person examination. As long as the doctor has a pre-existing relationship with the patient, prescribing is also appropriate for telephone consultations.
3. Informing the patient
Certain states in the United States of America have results and regulations that require doctors or healthcare experts to inform patients about the use of telemedicine. However, whether your state requires it or not, it is an excellent practice. Before the first telemedicine consultation or appointment, your doctor or the clinic will clarify the patient regarding the functioning of telemedicine software, such as when service is available, privacy, scheduling, and other details. Everything should be described or explained in easy-to-understand and straightforward language.
4. Set-up the right space for telemedicine visits
Doctors should build a specific area to access telemedicine to establish anonymity, lightning, prevent interruptions, and clear audio. Healthcare providers will place their cameras on a specific level stand and aim them at eye level.
Read Also: What is Telemedicine Services and How does it work?
How Does Telemedicine Work?
While you were reading this a question is clicking in your head that how does telemedicine software works. Below is
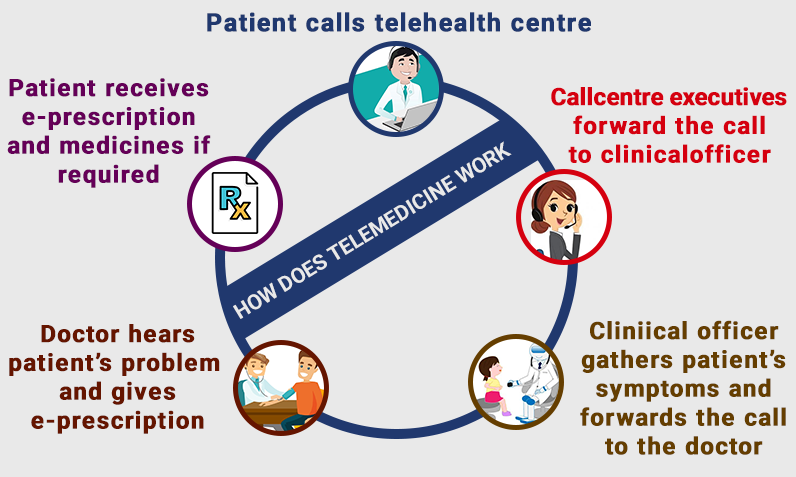
|
How is Telemedicine Impacting the Global Healthcare Trends?
Inequitable distribution of health professionals: Most health service providers live and work in large urban centres. This contributes to the acute shortage of health professionals in many smaller communities and rural areas where the provision of equitable access to health services is increasingly challenging.
1. An ageing population:
As the healthcare environment resumes to improve, this means patients will continue to receive better care over time. Because of this, global average life expectancy rates are rising. Facilities need to make moves to help relieve providers of the strain that comes with treating more patients.
2. Shortage of health professionals:
There is a general shortage of healthcare professionals. That threatens the provision of some healthcare services and extends the waiting lists.
3. Limited integration:
Care silos fail to provide timely and easy access for patients and providers to the information they need and cause delays and excessive duplication of service.
4. Fragmented funding:
Health service funding is a complicating factor, and is currently a matter of intense scrutiny and considerable controversy. The separation of political, managerial and fiscal responsibility across provincial and federal lines has generated tensions particularly around the issue of the current level, and the most acceptable level of potential funding.
5. Budget constraints:
New therapies and technologies are costing more and putting additional demands on the budgets of stressed health care.
6. Increasing cases of chronic conditions:
Did you know that chronic disease is responsible for 70 per cent of deaths every year in the U.S. alone? Patients have historically only had the option to visit doctors by in-person appointments, but many of today’s chronic illnesses are avoidable or treatable by doctors using video appointments to “check-in” and monitor patient’s remotely.
What Services Telemedicine Offer
You must be wondering what services must be provided by Telemedicine; well it can be used for a wide variety of health services. Telemedicine services can range widely by specialty. An endocrinologist might use it for doing a video call with patients, dentists can use it to encourage preventive care and appropriate follow-up, and a gynecologist might use it to provide birth control counseling.
Below is a list of common conditions a primary care doctor may treat via telemedicine:
- Cold and Flu
- Skin Treatments and Infections
- Infection
- Food poisoning
- Sprains and Strains
- Throat infections
- Allergies
- Counseling
- Rashes
- UTIs
- Human Immunodeficiency Virus
- Tuberculosis
- Hepatitis C Virus
HIPAA and Telemedicine

HIPAA stands for Health Insurance Portability and Accountability Act, which is designed to protect patients’ medical record and other health information. Like all the technologies in the healthcare industry, telemedicine software need to be in compliant with HIPPA in order to protect patient’s privacy. There are certain rules and regulations applied by HIPAA Security Rule on Telemedicine.
Conclusion
Are you the one, who are looking for HIPAA Compliant Telemedicine app Development Company?
We can Help!
Dreamsoft4u Pvt. Ltd. is one of the Best Telemedicine Companies in India and the USA. We maintained a highly favorable rating among dentists, physicians, and patients.
We have client range from dental clinics, hospitals, rural clinics, blood processing agencies, individual physician, and full-service hospitals. We offer planning, system integrations migrations, and many more. Our Healthcare IT Solutions make your staff hassle-free so they can focus on patient and client requirements.












